A common cause of lower leg and back pain is a ruptured disc or herniated disc. Symptoms of a herniated disc may include muscle spasm or cramping sharp or dull pain, sciatica, and leg weakness or loss of leg work. Sneezing, coughing, or bending intensify the pain.
Rarely, bowel or bladder control is lost, and when this happens, seek medical attention at once.
Sciatica is a symptom often associated with a lumbar herniated disc. Stress on one or several nerves that contribute to the sciatic nerve can lead to pain, burning, tingling, and numbness that extends from the buttocks into the leg and into the foot. Normally one side (left or right) is affected.
Anatomy of Lumbar Spine Discs
First, a brief overview of spinal anatomy so that you can better understand the way the lumbar herniated disc may lead to lower back pain and leg pain.
In between each of the 5 lumbar vertebrae (bones) is a disc, a tough, fibrous shock-absorbing pad. Endplates line the endings of every vertebra and help hold discs in place. Every disc includes a tire-like outer ring (annulus fibrosus) that encases a gel-like material (nucleus pulposus).
Disc herniation occurs when the annulus fibrous breaks open or cracks, permitting the nucleus pulposus to escape. Though you may have heard it be called a ruptured disc or even a bulging disc, this is called a herniated nucleus pulposus or herniated disc.
When a disc herniates, it can press on the spinal cord or spinal nerves. All along your spine, nerves are branching off from the spinal cord and travelling to various parts of your body. The nerves pass through small passageways between the vertebrae and discs, so if a herniated disc presses into that passageway, it can compress (or “pinch”) the nerve. This can result in the pain associated with herniated discs. (In the case below, you can observe a close-up look at a herniated disc pressing on a spinal nerve.)
Lumbar Herniated Disc Risk Factors
Many factors can increase the risk for disc herniation, including:
- Lifestyle choices like tobacco use, lack of regular exercise, and insufficient nourishment significantly contribute to inadequate disc health.
- As the body ages, natural chemical modifications cause discs to slowly dry out, which can impact disc strength and resiliency. To put it differently, the aging process can make your discs less capable of absorbing the shock from the body’s movements, which is one of their most important jobs.
- Poor posture combined with the habitual use of incorrect body mechanics stresses the lumbar spine and influences its usual ability to take the bulk of the body’s weight.
Combine these factors with the eeffects from daily wear and tear, injury, incorrect lifting, or twisting and it is simple to comprehend why a disc may herniate. For example, lifting something incorrectly may lead to disc pressure.
Disc Herniation Phases
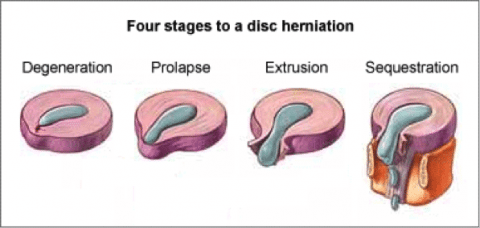
A herniation may develop suddenly or slowly over weeks or months. The four phases to a herniated disc are:
1) Disc Degeneration: Chemical modifications related to aging causes discs to weaken, but with no herniation.
2) Prolapse: The form or position of the disc changes with a few small impingement into the spinal canal and/or spinal nerves. This stage is also referred to as a bulging disc or a disc that was protruding.
3) Extrusion: The gel-like nucleus pulposus breaks through the tire-like wall (annulus fibrosus) but remains within the disc.
4) Sequestration or Sequestered Disc: The nucleus pulposus fractures throughout the annulus fibrosus and can then go outside the intervertebral disc.
Lumbar Herniated Disc Diagnosis
Lately, not every herniated disc causes symptoms. Some people discover they have a ruptured disc or herniated disc after an x-ray for an unrelated reason.
Most of the time, the symptoms, notably the pain, prompt the patient to seek medical attention. The trip with the doctor includes a physical exam and neurological exam. He or she will examine your medical history, and inquire about what remedies you have tried for pain relief and what symptoms you’ve experienced.
An x-ray may be needed to rule out other causes of back pain like osteoarthritis (spondylosis) or spondylolisthesis. A CT or MRI scan verifies the extent and location of disc damage.These imaging tests can show the soft tissues (including the disc).
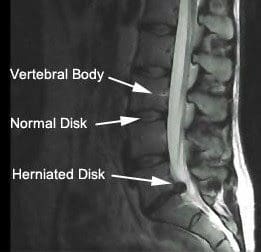
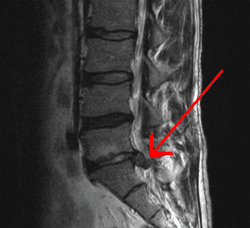
Sometimes a myelogram is essential. In that evaluation, you will receive an injection of a dye; the dye will appear on a CT scan, so allowing your physician to readily see problem areas.
The scope of our information is limited to chiropractic and spinal injuries and conditions. To discuss options on the subject matter, please feel free to ask Dr. Jimenez or contact us at 915-850-0900 . 
By Dr. Alex Jimenez
Additional Topics: Sciatica
Lower back pain is one of the most commonly reported symptoms among the general population. Sciatica, is well-known group of symptoms, including lower back pain, numbness and tingling sensations, which often describe the source of an individual’s lumbar spine issues. Sciatica can be due to a variety of injuries and/or conditions, such as spinal misalignment, or subluxation, disc herniation and even spinal degeneration.

TRENDING TOPIC: EXTRA EXTRA: New PUSH 24/7®? Fitness Center
Post Disclaimer *
Professional Scope of Practice *
The information herein on "Sciatica Specialist: Lumbar Herniated Disc Anatomy" is not intended to replace a one-on-one relationship with a qualified health care professional or licensed physician and is not medical advice. We encourage you to make healthcare decisions based on your research and partnership with a qualified healthcare professional.
Blog Information & Scope Discussions
Welcome to El Paso's Premier Fitness, Injury Care Clinic & Wellness Blog, where Dr. Alex Jimenez, DC, FNP-C, a Multi-State board-certified Family Practice Nurse Practitioner (FNP-BC) and Chiropractor (DC), presents insights on how our multidisciplinary team is dedicated to holistic healing and personalized care. Our practice aligns with evidence-based treatment protocols inspired by integrative medicine principles, similar to those found on this site and our family practice-based chiromed.com site, focusing on restoring health naturally for patients of all ages.
Our areas of multidisciplinary practice include Wellness & Nutrition, Chronic Pain, Personal Injury, Auto Accident Care, Work Injuries, Back Injury, Low Back Pain, Neck Pain, Migraine Headaches, Sports Injuries, Severe Sciatica, Scoliosis, Complex Herniated Discs, Fibromyalgia, Chronic Pain, Complex Injuries, Stress Management, Functional Medicine Treatments, and in-scope care protocols.
Our information scope is multidisciplinary, focusing on musculoskeletal and physical medicine, wellness, contributing etiological viscerosomatic disturbances within clinical presentations, associated somato-visceral reflex clinical dynamics, subluxation complexes, sensitive health issues, and functional medicine articles, topics, and discussions.
We provide and present clinical collaboration with specialists from various disciplines. Each specialist is governed by their professional scope of practice and their jurisdiction of licensure. We use functional health & wellness protocols to treat and support care for musculoskeletal injuries or disorders.
Our videos, posts, topics, and insights address clinical matters and issues that are directly or indirectly related to our clinical scope of practice.
Our office has made a reasonable effort to provide supportive citations and has identified relevant research studies that support our posts. We provide copies of supporting research studies upon request to regulatory boards and the public.
We understand that we cover matters that require an additional explanation of how they may assist in a particular care plan or treatment protocol; therefore, to discuss the subject matter above further, please feel free to ask Dr. Alex Jimenez, DC, APRN, FNP-BC, or contact us at 915-850-0900.
We are here to help you and your family.
Blessings
Dr. Alex Jimenez DC, MSACP, APRN, FNP-BC*, CCST, IFMCP, CFMP, ATN
email: [email protected]
Multidisciplinary Licensing & Board Certifications:
Licensed as a Doctor of Chiropractic (DC) in Texas & New Mexico*
Texas DC License #: TX5807, Verified: TX5807
New Mexico DC License #: NM-DC2182, Verified: NM-DC2182
Multi-State Advanced Practice Registered Nurse (APRN*) in Texas & Multi-States
Multistate Compact APRN License by Endorsement (42 States)
Texas APRN License #: 1191402, Verified: 1191402 *
Florida APRN License #: 11043890, Verified: APRN11043890 *
Verify Link: Nursys License Verifier
* Prescriptive Authority Authorized
ANCC FNP-BC: Board Certified Nurse Practitioner*
Compact Status: Multi-State License: Authorized to Practice in 40 States*
Graduate with Honors: ICHS: MSN-FNP (Family Nurse Practitioner Program)
Degree Granted. Master's in Family Practice MSN Diploma (Cum Laude)
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)
(Licensed Medical Doctor)
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933
Licenses and Board Certifications:
MD: Medical Doctor
DC: Doctor of Chiropractic
APRNP: Advanced Practice Registered Nurse
FNP-BC: Family Practice Specialization (Multi-State Board Certified)
RN: Registered Nurse (Multi-State Compact License)
CFMP: Certified Functional Medicine Provider
MSN-FNP: Master of Science in Family Practice Medicine
MSACP: Master of Science in Advanced Clinical Practice
IFMCP: Institute of Functional Medicine
CCST: Certified Chiropractic Spinal Trauma
ATN: Advanced Translational Neutrogenomics
Memberships & Associations:
TCA: Texas Chiropractic Association: Member ID: 104311
AANP: American Association of Nurse Practitioners: Member ID: 2198960
ANA: American Nurse Association: Member ID: 06458222 (District TX01)
TNA: Texas Nurse Association: Member ID: 06458222
NPI: 1205907805
| Primary Taxonomy | Selected Taxonomy | State | License Number |
|---|---|---|---|
| No | 111N00000X - Chiropractor | NM | DC2182 |
| Yes | 111N00000X - Chiropractor | TX | DC5807 |
| Yes | 363LF0000X - Nurse Practitioner - Family | TX | 1191402 |
| Yes | 363LF0000X - Nurse Practitioner - Family | FL | 11043890 |
| Yes | 363LF0000X - Nurse Practitioner - Family | CO | C-APN.0105610-C-NP |
| Yes | 363LF0000X - Nurse Practitioner - Family | NY | N25929 |
Dr. Alex Jimenez, DC, APRN, FNP-BC*, CFMP, IFMCP, ATN, CCST
(Board Certified: Family Practice Nurse Practitioner—Multistate)*
(Licensed Nurse Practitioner & Chiropractor - Multistate)*
Clinical Director
Digital Business Card
Dr. Maria Cardenas, MD
(Board Certified: Internal Medicine)*
(Licensed Medical Doctor)*
Medical Director, Clinical Director & Collaborative Physician
NPI # 1164426749
MD License #: J2933



